What to engrave on MedicAlert medical IDs for organ transplant:
MedicAlert offers free custom engraving on all our organ transplant bracelets and medical ID products. Engravings on medical IDs for organ transplant should include any critical medical information that can protect and save your life if you are in an accident or have a medical emergency, for example:
- Type and date of organ transplant
- Medications you’re taking, especially anti-rejection meds or other immunosuppressants
- If you are a living organ donor, indicate the missing organ
- Allergies
- Other medical conditions that might or might not be connected to the organ transplant, such as chronic kidney disease, diabetes, or heart disease
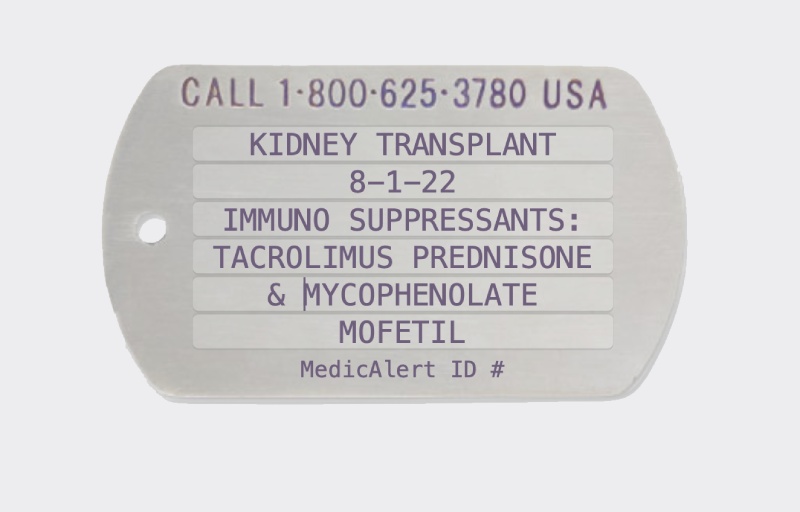
Sample engraving. Consult our team if you need help engraving your medical ID for organ transplant.












